Just one lung should be had to function relatively normally still.
Since the lungs are essential organs in the body, specific disorders may result in a person losing function in their lungs or having to remove one.
That said, each entity would be different, and in each case based on the lung capacity of the person and any other complications they face, there are special considerations.
To learn more, carry on reading.
Can you survive with one lung?
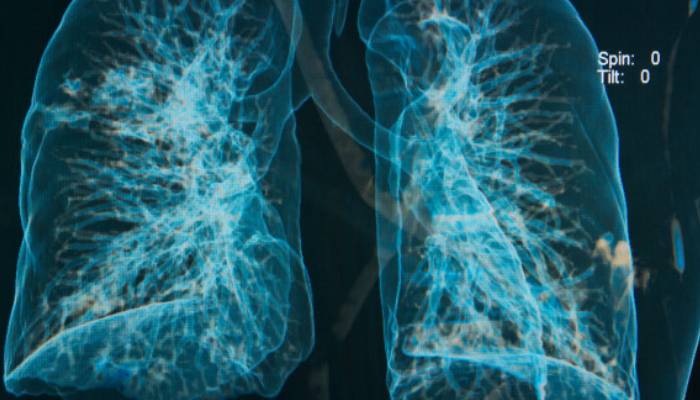
The lungs are the human body’s essential organs, responsible for bringing oxygen into the body and helping with every exhale to get rid of waste gases.
While having both lungs is preferable, without one lung, it is possible to survive and work. Having one lung will still make it possible for an individual to live a relatively everyday life.
Having one lung could, however, restrict the physical abilities of a person, such as their ability to exercise. That said, many athletes will still practice and be able to pursue their sport if they lose the use of one lung.
In many ways, the body adapts to this transition. The remaining lung, for example, will extend a little to fill the space vacated by the absent lung. The body will also learn over time to make up for oxygen loss.
However, as with two lungs, a person will not have the full lung capacity, and they will probably need to learn to slow down and adapt to this change.
While most individuals expect to be winded continuously or to have an inability to function without one lung, this is usually not what happens. The individual may have to learn to slow down their normal functions to a degree, but with one lung, they should be able to lead a relatively everyday life.
Risks and dangers
While surviving without a lung is feasible, there are a lot of risks involved.
Pneumonectomy, or operation to cut one of the lungs, is a high-risk surgery that may lead to complications and even death, a report in the Journal of Cancer reports.
Possible pneumonectomy-related complications include:
Breathing Loss
Shock and unnecessary bleeding
Abnormal rhythms of the heart, or arrhythmia
Diminished blood supply
Pulmonary embolism, or blood clots in the lungs
Pneumonia
The anesthetic from the procedure often bears its risks.
The internal method of pneumectomy includes making an incision to remove the infected lung from the side of the body.
The void left after the lung is replaced will be filled with air. An individual may experience transient abdominal pain or pressure during healing as this air shifts and assimilates into the body. The other lungs will grow a bit over time and fill up more of this area. Naturally, the room left would fill up with fluid.
An individual will also take a while to recover after a successful procedure. Complete recovery can take weeks or even months without complications.
The participant will need to be mindful of their limits when healing and even after, and will have to reduce their levels of operation drastically.
Any factors can make a person feel windier, placing them at risk of diminished blood pressure or fainting. Also, daily tasks can cause the person to feel very windy, such as getting out of bed in the morning, standing up from a prone position, or walking upstairs.
Additional variables may also play into the risk of an individual. For example, their general health could affect their risks before the surgery, their age, and any other health conditions they have.
It would be essential to be extra vigilant for people with a history of smoking or other lung disorders that restrict their lung capacity. During recovery, they may require medical help and should consult closely with a specialist to consider their complications.
Why you will need a removed lung

The most common reason is lung cancer. It’s typically cancer that starts in the lungs, but as cancers reach out from another area of the body, it could also happen.
Not everyone with lung cancer is going to need to lose a lung. For individuals with tumors that are extremely large or develop near the center of the lung, it may be an alternative.
During a pneumonectomy, what happens?
For the surgery, you’ll get drugs to bring you absolutely to sleep.
A surgeon who wants removal will slash into the side of your chest nearest to the lung. Your lung would fail, blocking the wider blood vessels surrounding it, cutting the central bronchial canal as close as possible to the windpipe, and destroying the lung.
They will then close what remains of the cut bronchial tube to ensure the air does not escape.
The surgeon will also strip the lining of your chest wall (called the pleura) together with sections of other surrounding tissue in an’ extrapleural’ pneumonectomy, and patch them with reliable, clean, human-made materials.
After a Pneumonectomy, what happens?
Usually, after surgery, you will continue to stay in the hospital for a week or two so that the medical provider can monitor your heart rate, pulse, and blood pressure and monitor you for infection.
You shouldn’t have significant discomfort, but you might be sore. Tell your doctor if you have a feeling, mainly if it unexpectedly happens.
To practice special breathing techniques, you can consult with a qualified specialist called a respiratory therapist, who you may need to do a few times a day. Both help you improve your breathing and extract fluid from the surgery that builds up.
In the first few days, you will need someone to take you home from the hospital and support you around the building. Initially, take it easy—no heavy lifting. You can get exhausted more quickly, but within the next few weeks or months, your strength and endurance can return.
READ THIS NEXT
The Fast Metabolism Diet For Lose Weight
Benefits of Using Conditioner Before Shampoo
How to Drink Matcha Tea for Weight Loss

Comments are closed.